Perfusion Case Study 1
An 89-year old female client is admitted to a telemetry unit with a diagnosis of heart failure exacerbations. She reports a medical history of osteoarthritis, chronic lymphocytic leukemia, and coronary artery disease including a myocardial infarction and coronary artery bypass surgery 22 years ago. She is alert and her daughter is at her bedside.
Results for question 1.
11 / 1 point
Multiple answer
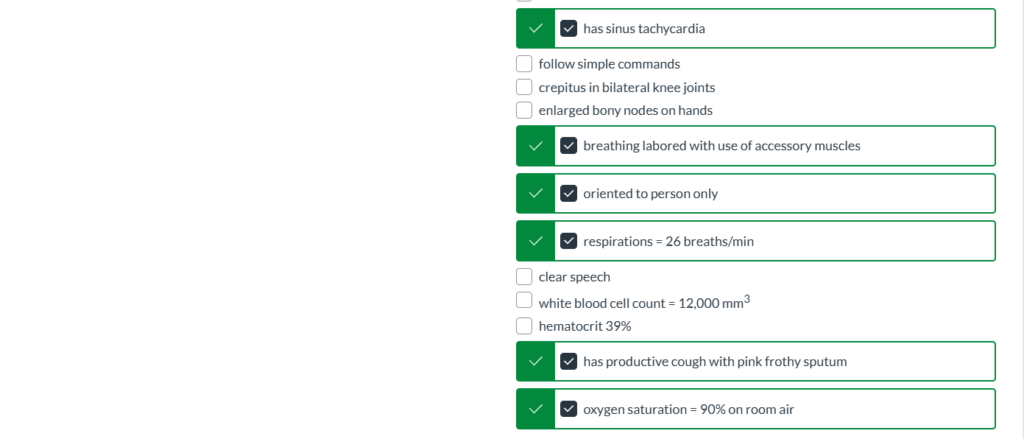
The nurse’s initial client assessment findings include the following. Which assessment findings require follow-up by the nurse? Select all that apply.
Answer,
hemoglobin 12.4 g/dL
Correct answer:
has sinus tachycardia
Answer,
follow simple commands
Answer,
crepitus in bilateral knee joints
Answer,
enlarged bony nodes on hands
Correct answer:
breathing labored with use of accessory muscles
Correct answer:
oriented to person only
Correct answer:
respirations = 26 breaths/min
Answer,
clear speech
Answer,
white blood cell count = 12,000 mm3
Answer,
hematocrit 39%
Correct answer:
has productive cough with pink frothy sputum
Correct answer:
oxygen saturation = 90% on room air
Feedback
Based on answering correctly
Coronary artery disease is a common risk factor for ventricular dysfunction and heart failure. Confusion or orientation to person only should alert the nurse to impaired cerebral perfusion, a complication of inadequate cardiac output. Although the client is an older adult, the nurse cannot assume that the client’s impaired orientation is related to age and must complete additional assessments to identify the cause. Sinus tachycardia is a manifestation of compensation for inadequate cardiac output, infection, or other physiologic issues. The nurse must follow-up on this symptom based on the client’s previous cardiac disease, which increases the client’s risk for hypoxemia. An increase in heart rate creates an increased demand for oxygen by the myocardium, which can lead to angina and cardiac arrest. The oxygen saturation, dyspnea and labored breathing, and pink frothy sputum are symptoms of pulmonary congestion. When these symptoms are present, the nurse must intervene early to prevent an acute pulmonary edema episode, which could lead to respiratory failure. Crepitus in bilateral knee joints and enlarged bony nodes on hands are manifestations of osteoarthritis, are not acute symptoms, and do not require follow-up at this time. The client’s white blood count is a little high and is likely a manifestation of the client’s chronic lymphocytic leukemia.
Results for question 2.
21 / 1 point
Categorisation
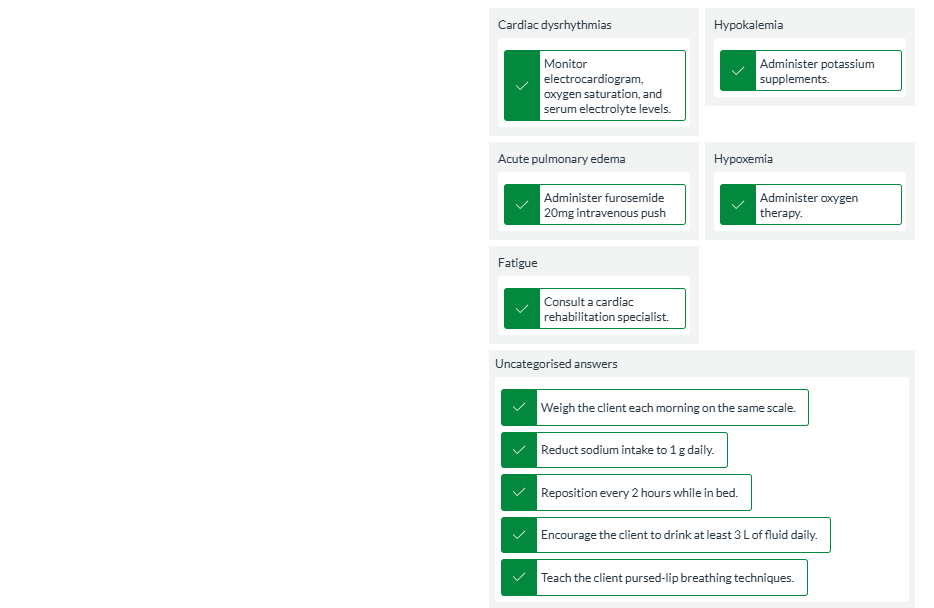
Indicate which nursing action listed is most appropriate for each potential heart failure complication. Each complication will have one (1) action. Note: not all actions will be used.
CategoryCardiac dysrhythmias
Correct answer:
Monitor electrocardiogram, oxygen saturation, and serum electrolyte levels.
CategoryHypokalemia
Correct answer:
Administer potassium supplements.
CategoryAcute pulmonary edema
Correct answer:
Administer furosemide 20mg intravenous push
CategoryHypoxemia
Correct answer:
Administer oxygen therapy.
CategoryFatigue
Correct answer:
Consult a cardiac rehabilitation specialist.
Uncategorised answers
Correct answer:
Weigh the client each morning on the same scale.
Correct answer:
Reduct sodium intake to 1 g daily.
Correct answer:
Reposition every 2 hours while in bed.
Correct answer:
Encourage the client to drink at least 3 L of fluid daily.
Correct answer:
Teach the client pursed-lip breathing techniques.
Feedback
Based on answering correctly
Acute pulmonary edema is an emergent situation and requires the nurse to implement care immediately in order to prevent respiratory failure. Rapid-acting diuretics such as furosemide, are administered via intravenous push to remove fluid from the body, specifically from the alveoli, to improve oxygenation and perfusion. Fatigue is a common manifestation of heart failure, secondary to decreased cardiac output, impaired tissue perfusion, and anaerobic metabolism, and leads to activity intolerance. Consulting a cardiac rehabilitation specialist who can focus on balancing client activity with symptoms of exertion will help the client to begin rehabilitation activities while in the hospital. Hypokalemia is a common side effect of diuretic treatments prescribed for clients experiencing pulmonary congestion. Monitoring serum electrolyte levels will assist the nurse in identifying hypokalemia, but the administration of potassium supplements is necessary to ensure that levels remain within normal ranges. Irregular heart rhythms from premature atrial contractions, premature ventricular contractions, or atrial fibrillation are common in clients with heart failure. Cardiac dysthythmias result from myocardial ischemia, pulmonary hypertension, valvular disease, sympathomimetic agents, and electrolyte imbalances, specifically hypokalemia and hypomagnesemia. The nurse would closely monitor serum electrolyte levels, oxygenation saturation, and other vital signs to identify potential causes of dysrhythmias early. The client would also have continuous electrocardiogram monitoring. Hypoxemia is a complication of inadequate oxygen diffusion secondary to pulmonary congestion, and impaired cardiac output related to ventricular dysfunction. Providing supplemental oxygen increases the amount of oxygenated blood available to organs throughout the body. Oxygen should be administered via mask as needed to keep oxygen saturation levels greater than 90%. Repositioning the client every 2 hours while in bed improves gas exchange and prevents skin breakdown but does not address the client’s oxygen needs nor the client’s fatigue with ADLs.
Results for question 3.
31 / 1 point
Multiple answer
The client is scheduled to be discharged today and will move in with her daughter until she feels well enough to go home alone. Which of the following discharge instructions will the nurse provide the client and her daughter? Select all that apply.
Answer,
“Heart failure is a chronic condition, so you don’t need to be alarmed when you experience heart palpitation.”
Correct answer:
“Do not use table salt. Avoid salty foods and read labels on all food items to ensure your diet is low in sodium.”
Correct answer:
“Weigh yourself each day at the same time on the same sale to monitor for fluid retention.”
Correct answer:
“Notify your primary health care provider if you experience shortness of breath or chest pain while resting.”
Correct answer:
“Contact your primary health care provider if you experience cold symptoms lasting more than 3 days.”
Answer,
“Exertion can cause another episode of heart failure, so help your mother by performing daily activities for her.”

Feedback
Based on answering correctly
Changes in weight over a short period of time indicate changes in the body’s fluid volume. Clients who have heart failure are taught to weigh themselves every day to monitor for fluid changes, especially fluid retention. Clients are taught to contact the primary health care provider immediately if they experience a rapid weight gain of 3 lb in 1 week or 1 to 2 lb in 1 day, as this is a sign of recurrent heart failure. Clients with heart failure are taught to contact the primary health care provider when experiencing cold symptoms including a cough that lasts more than 3 to 5 days. Symptoms that a client associates with a cold may be a sign of worsening heart failure. Clients with heart failure frequently experience dyspnea and may sometimes experience chest pain with activity and exertion. Both shortness of breath and chest pain should resolve with rest. Experiencing dyspnea or angina while at rest is a sign of a heart failure exacerbation. The client must be taught to contact the primary health care provider if these symptoms occur. Although the client may experience shortness of breath with activity, the client is encouraged to maintain independence when performnd ADLs. Therefore the client’s daughter should not be taught to perform activities for her mother. Decreasing salt intake will reduce fluid retention by the kidneys. Clients with heart failure are taught to avoid salty foods and table salt and how to read food labels for sodium content. Heart palpitations are a compliation of heart failure, and the client should be taught to contact the primary health care provider if this symptom occurs.
Results for question 4.
41 / 1 point
Categorisation
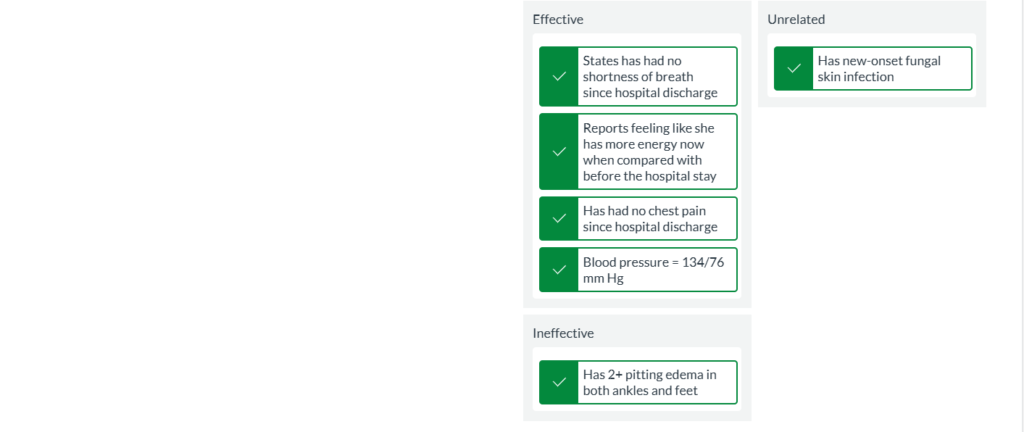
The client was discharged 2 weeks ago and is with her daughter for her follow-up primary health care provider visit. For each assessment finding, drag the cue to the correct category: effective (helped to meet expected outcomes), ineffective (did not help to meet expected outcomes), or unrelated (not related to the expected outcomes).
CategoryEffective
Correct answer:
States has had no shortness of breath since hospital discharge
Correct answer:
Reports feeling like she has more energy now when compared with before the hospital stay
Correct answer:
Has had no chest pain since hospital discharge
Correct answer:
Blood pressure = 134/76 mm Hg
CategoryUnrelated
Correct answer:
Has new-onset fungal skin infection
CategoryIneffective
Correct answer:
Has 2+ pitting edema in both ankles and feet

Feedback
Based on answering correctly
The client was admitted to the hospital with fluid overload, dyspnea, and fatigue, which are all common symptoms of heart failure. Now she reports that she has no shortness of breath and has more energy. Therefore the interventions worked to manage her disease. Her blood pressure is likely within usual parameters for her advanced age, and she has no chest pain, indicating successful management of her health. However, she continues to have some fluid overload as evidenced by ankle and foot edema. Having a fungal skin infection is not related to teh client’s current or previous medical diagnoses.
Perfusion Case Study 2
A 69-year-old female client is participating in acute rehabilitation after a vehicular accident that resulted in a fractured arm, fractured clavicle, and several fractured ribs. The client has no recorded medical history. She claims to be healthy and only sees her primary health care provider every few years.
Results for question 5.
51 / 1 point
Multiple answer
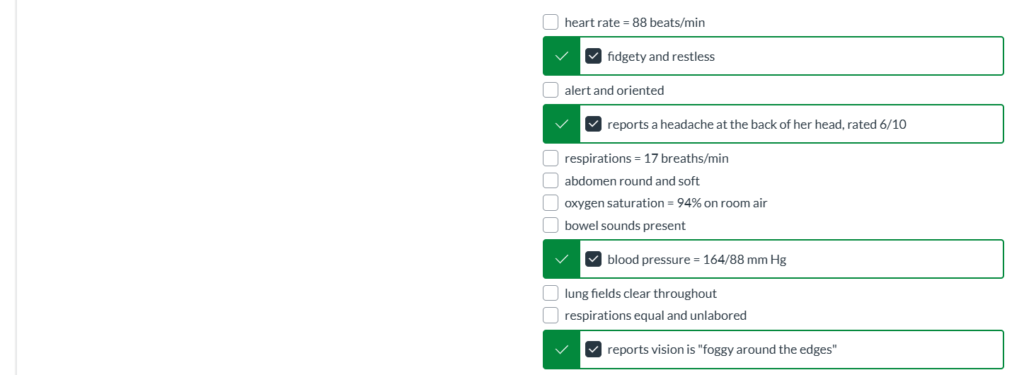
Client findings from the nurse’s shift assessment include the following. Which require follow-up by the nurse in collaboration with the health care team? Select all that apply.
Answer,
heart rate = 88 beats/min
Correct answer:
fidgety and restless
Answer,
alert and oriented
Correct answer:
reports a headache at the back of her head, rated 6/10
Answer,
respirations = 17 breaths/min
Answer,
abdomen round and soft
Answer,
oxygen saturation = 94% on room air
Answer,
bowel sounds present
Correct answer:
blood pressure = 164/88 mm Hg
Answer,
lung fields clear throughout
Answer,
respirations equal and unlabored
Correct answer:
reports vision is “foggy around the edges”
Feedback
Based on answering correctly
The client’s restless behavior may be a sign of anxiety. There are many reasons the client could be feeling anxious, and the nurse must complete a more thorough assessment to determine the cause. Pain must always be assessed completely. Headaches can have a variety of causes including some life-threatening conditions. A headache with an accomopanying report of vision changes is especially concerning, and the nurse must urgently follow-up on these symptoms. The client’s vital signs are within normal limits with the exception of the blood pressure, which is elevated. Because the nurse does not know the client’s health history, it is essential for the nurse to follow-up on the blood pressure to determine if it is related to acute pain and anxiety or to another primary problem that is causing the client’s headache, visual changes, and anxious feelings. The other client findings are all within usual limits.
Results for question 6.
61 / 1 point
Multiple answer
The nurse further assesses the client for risk factors of potential health issues associated with the above findings. What additional information does the nurse need to analyze the client’s findings. Select all that apply.
Correct answer:
usual sleep cycle
Correct answer:
usual dietary intake
Correct answer:
history of migraines or headaches
Answer,
peripheral pulses
Correct answer:
facial symmetry
Correct answer:
pupil size and reaction
Answer,
recent immunizations
Correct answer:
smoking history

Feedback
Based on answering correctly
Headache, vision changes, and anxiety are associated with life-threatening conditions including stroke and intracranial hemorrhage. The nurse needs to complete a thorough neurologic assessment to determine if the client has any additional signs of these disorders. The nurse assesses the client’s cranial nerves, including pupils for size, shape, and reaction and facial movement for symmetry. Because the nurse knows little about the client’s health history, the nurse will also ask questions to obtain more informtion about the client’s health status and healthy or risky behaviors. Questions focused on nutrition, exercise, sleep, and stress will help the nurse to identify health risks. Questions focused on use of nicotine, alcohol, and other substances must also be asked. Finally, the nurse will assess for any history of headaches or migraines, because visual changes may accompany migraine headaches. Assessing peripheral pulses and recent immunizations will not assist the nurse in analyzing cues and identifying priority client needs.
Results for question 7.
71 / 1 point
Categorisation
The client works as a retail cashier and is the primary caregiver for her two school-age grandchildren. She usually eats fast foods, sleeps only 4-5 hours a night, and drinks many caffeinated beverages to “keep going”. The client reports a 21-pack-year history of cigarette smoking. Current findings include signs of anxiety and visual changes but no neurologic deficits. The client also reports an occipital headache, rated 6/10 on a 0 to 10 scale, and has a blood pressure of 164/88 mm Hg. The client is diagnosed with hypertension.
The nurse collaborated with the health care team to revise the client’s plan of care. Drag and drop the nursing interventions to show whether each nursing action is indicated (appropriate or necessary), contraindicated (could be harmful), or non-essential (makes no difference or is not necessary) for the client’s care at this time.
CategoryNon-Essential
Correct answer:
Ensure naloxone is on the unit in case of an overdose of antihypertensive medications.
CategoryContraindicated
Correct answer:
Collaborate with a physical therapist for passive range-of-motion activities when orthostatic hypotension occurs.
CategoryIndicated
Correct answer:
Provide client teaching focused on nutrition, exercise, and medication therapy.
Correct answer:
Monitor for therapeutic and side effects of antihypertensive medications.
Correct answer:
Consult a registered dietitian nutritionist to facilitate a low-fat and low-sodium diet.

Feedback
Based on answering correctly
Hypertension is a chronic disease that requires long-term management. Client education is critical for effective management and must be included in the client’s plan of care. The client’s immediate concerns and questions should be addressed first, followed by information on diet therapy, exercise, and medications. Goals of diet therapy for a client with hypertension are to maintain ideal body weight and prevent fluid retention. A low-fat and low-sodium diet would be implemented. The client will be started on new medications. The nurse must monitor the client for therapeutic and side effects of drug therapy to ensure that the client’s blood pressure is successfully lowered without negative symptoms. The nurse will collaborate with physical therapy and occupational therapy personnel to ensure that the client is safe during all acitvities. Antihypertensive medications increase the client’s risk for orthostatic hypotension, and passive range of motion would not be performed when blood pressure is low. The client should continue fully participating in therapies.
Results for question 8.
81 / 1 point
Multiple answer
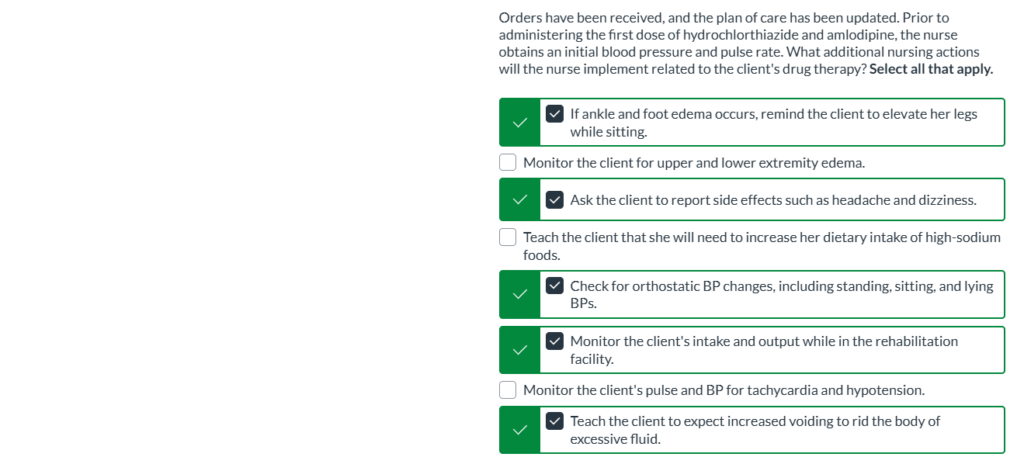
Orders have been received, and the plan of care has been updated. Prior to administering the first dose of hydrochlorthiazide and amlodipine, the nurse obtains an initial blood pressure and pulse rate. What additional nursing actions will the nurse implement related to the client’s drug therapy? Select all that apply.
Correct answer:
If ankle and foot edema occurs, remind the client to elevate her legs while sitting.
Answer,
Monitor the client for upper and lower extremity edema.
Correct answer:
Ask the client to report side effects such as headache and dizziness.
Answer,
Teach the client that she will need to increase her dietary intake of high-sodium foods.
Correct answer:
Check for orthostatic BP changes, including standing, sitting, and lying BPs.
Correct answer:
Monitor the client’s intake and output while in the rehabilitation facility.
Answer,
Monitor the client’s pulse and BP for tachycardia and hypotension.
Correct answer:
Teach the client to expect increased voiding to rid the body of excessive fluid.
Feedback
Based on answering correctly
The client is starting hydrochlorthiazide (HCTZ), a diuretic that is a first-line treatment for hypertension. This drug increases urinary output to rid the body of excessive fluid and decrease intravascular volume. The nurse would monitor the client’s intake and output to ensure fluid balance. Electrolytes would also be monitored because the HCTZ causes loss of sodium (desired to help lose excessive fluid) and postassium (not desired and must be replaced). Both HCTZ and amlodipine can cause dizziness and orthostatic blood pressure changes, requiring nurse monitoring. Side effects of amlodipine include bradycardia, hypotension, headache, and ankle and foot edema. If dependent edema occurs, the nurse would teach the client the need to elevate her lower extremities while sitting.
Results for question 9.
91 / 1 point
Categorisation
For each client statement, drag the statement to the correct category to indicate if teaching was effective (helped the client understand discharge teaching), ineffective (did not help the client understand discharge teaching), or unrelated (not related to discharge teaching).
CategoryUnrelated
Correct answer:
“I will take my pulse for a full minute prior to taking my antihypertensive medications.”
CategoryIneffective
Correct answer:
“Once my blood pressure is within normal limits, I can stop taking the medication.”
CategoryEffective
Correct answer:
“I will use the resources provided to begin a smoking cessation program.”
Correct answer:
“I will add more fruits and vegatables to my diet and eat less fast food.”
Correct answer:
“Spices, garlic, and onions can add flavor to my food without adding more sodium.”
Feedback
Based on answering correctly
Smoking aggravates hypertension, and therefore, clients with hypertension will be encouraged to quit. The nurse will provide the client with information about local resources including the American Heart Association’s smoking cessation programs. The nurse will help the client develop healthy eating habits based on a diet moderately low in sodium and low in fat. Eating more fruits and vegatables and low-fat dairy products can help the client to eat the prescribed diet. Seasoning foods with spices, garlic, and onions instead of salt may also assist the client in decreasing sodium intake. Antihypertensive medications should be takes as prescribed and not stopped unless instructed to do so by the primary health care provider. Suddenly stopping these drugs may cause the client’s blood pressure to rise rapidly. Although her antihypertensive medications will lower her heart rate, there is no need for the client to take her pulse for a full minute before taking the medications.
